Most dentures last between 5 and 10 years with proper care. The exact lifespan depends on the type of denture, the materials used, how well you maintain them, and how your mouth changes over time. Even a structurally sound denture can lose its fit as the jawbone naturally reshapes after tooth loss. Knowing when to replace your dentures protects your comfort, your oral health, and the function of your smile.
What Determines How Long Dentures Last?
What determines how long dentures last includes the quality of materials, the accuracy of the original fit, daily wear and care habits, and biological changes inside the mouth. No two patients will get the same number of years from the same denture.
The American Dental Association (ADA) recommends having dentures examined by a dental professional for possible replacement every 5 to 7 years. The American College of Prosthodontists (ACP) takes a more case-by-case approach, recommending replacement when specific red flags appear, such as chronic irritation under the base, the need for adhesive to keep them in place, or visible degradation of the appliance.
A systematic review published in The Journal of Prosthetic Dentistry found that complete dentures last an average of about 10 years, though many patients need adjustments well before that point. The key takeaway is that dentures do not fail all at once. They lose effectiveness gradually as the mouth changes around them.
We create custom partial and complete dentures at our Cinnaminson office and schedule follow-up visits to monitor fit over time.
How Bone Resorption Affects Denture Fit
The biggest reason dentures stop fitting well is bone resorption. After a tooth is removed, the jawbone in that area no longer receives the chewing forces that kept it strong. The body responds by gradually breaking down and absorbing the unused bone. A study published in the Indian Journal of Dentistry found that up to 25% of the surrounding bone can be lost in the first year after a tooth extraction.
This process does not stop after year one. Research shows that the most dramatic bone loss occurs in the first 3 to 6 months, with some patients losing 40% to 60% of bone width in that period. After the initial phase, resorption continues at a slower but steady rate of about 1% per year.
For denture wearers, this means the gum ridge that supports the denture is constantly changing shape. A denture that fit perfectly at delivery may feel noticeably looser within a year or two. The lower jaw tends to lose bone faster than the upper jaw, which is one reason many patients find that lower dentures become unstable sooner.
According to the CDC's 2024 Oral Health Surveillance Report, adults aged 75 and older retain an average of roughly 20 teeth, down from 27 at ages 20 to 34. This progressive tooth loss, combined with ongoing bone resorption, is why regular dental evaluations are so important for denture wearers in Cinnaminson and the surrounding Burlington County area.
Signs That Your Dentures Need to Be Replaced
Dentures rarely break overnight. The signs that replacement is needed tend to develop slowly over weeks or months. The ACP's 2015 position statement (reaffirmed in 2018) outlines several red flags that signal a denture may need replacement.
Persistent looseness or slipping is one of the most common signs. If your denture moves when you eat, speak, or laugh, the underlying bone has likely changed enough that a reline or new denture is needed.
Chronic sore spots or irritation under the denture base can indicate poor fit. A review documented in The Journal of the American Dental Association found that wearing dentures longer than five years was associated with an increased risk of soft-tissue lesions. Ill-fitting dentures create pressure points that can lead to painful ulcers or even a condition called epulis fissuratum, where excess tissue grows in response to chronic friction.
Visible cracks, chips, or worn-down teeth on the denture itself are another clear signal. Denture teeth wear down from years of chewing, and structural damage like fractures or warping of the base affects both comfort and function.
If you need to use increasing amounts of denture adhesive to keep your denture stable, that is a sign the fit has changed and professional evaluation is overdue.
Patients throughout Cinnaminson, Moorestown, and Delran who notice any of these changes should schedule a visit so we can evaluate the fit and recommend the right next step.
| Denture Type | Average Lifespan | Key Factors Affecting Longevity |
|---|---|---|
| Complete (full) dentures | 5 to 10 years | Bone resorption rate, daily care, material quality |
| Partial dentures | 5 to 7 years | Health of anchor teeth, framework material, gum changes |
| Immediate dentures | 6 to 12 months (temporary) | Rapid bone and gum changes during healing |
| Implant-supported dentures | 10 to 15+ years | Implant health, bone density, maintenance schedule |
Sources: American Dental Association, American College of Prosthodontists, The Journal of Prosthetic Dentistry
Immediate dentures are placed the same day teeth are extracted. They serve as a temporary solution while the gums heal and the bone reshapes, which is why they typically need to be replaced or significantly relined within the first year.
Partial dentures depend on the health of the remaining natural teeth that serve as anchors. If an anchor tooth develops decay or gum disease and needs to be extracted, the partial may need to be redesigned or replaced entirely.
We offer both complete and partial denture solutions and can help you understand which type is right for your situation.
How Relining Extends Denture Life
Relining is a procedure that reshapes the inner surface of a denture to match the current contour of your gums. It is one of the most effective ways to extend the life of a denture that is still structurally sound but no longer fits snugly.
There are two types of relines. A hard reline uses the same type of acrylic as the original denture base and creates a durable, long-lasting adjustment. A soft reline uses a pliable material that provides a cushion between the denture and the gums, which can be helpful for patients with sore or sensitive tissue.
Most patients benefit from a reline every one to two years. The ACP's evidence-based guidelines note that relining is appropriate when the vertical dimension, occlusion, and overall function of the denture are still acceptable, but the tissue fit has changed.
Relining is not a permanent fix. As bone resorption continues, there comes a point where the denture base itself is too worn or too thin to support another reline. At that stage, a new denture is the better option.
South Jersey residents who feel their dentures loosening can visit our Cinnaminson dental office to find out whether a reline or replacement is the right call.
Daily Care Habits That Protect Your Dentures
Good daily care is the single most controllable factor in how long your dentures last. The ADA and the ACP published joint evidence-based guidelines recommending specific care practices to maximize denture lifespan and protect oral health.
Remove your dentures every night. The ACP guidelines specifically state that dentures should not be worn continuously for 24 hours, as doing so increases the risk of denture stomatitis, a fungal infection of the tissue beneath the denture. Removing them at night gives your gums time to rest and recover.
Clean your dentures daily by brushing them with a soft-bristled brush and a non-abrasive denture cleanser. Never use regular toothpaste, as it is too abrasive for acrylic and creates microscopic scratches that harbor bacteria. The ACP also recommends having dentures professionally cleaned with an ultrasonic cleanser at least once a year.
When dentures are not in your mouth, store them in water. Acrylic can warp if it dries out. Never place dentures in boiling water or soak them in bleach solutions for more than 10 minutes, as both can damage the material.
Patients who wear removable partial dentures also need to brush and floss their remaining natural teeth carefully. Decay in an anchor tooth can compromise the entire partial.
The Health Consequences of Wearing Old Dentures
Wearing dentures that no longer fit properly does more than cause discomfort. It can create real health problems over time.
According to the CDC, tooth loss can lead to poor diet, low self-esteem, difficulty speaking, and overall lowered quality of life. Dentures that do not fit well make these problems worse because they limit the types of food a person can chew comfortably. A National Institutes of Health report found that denture wearers face a 1.7 times greater risk of malnutrition compared to adults with a full natural set of teeth.
Ill-fitting dentures can also accelerate bone loss. When a denture rocks or shifts during chewing, it creates uneven pressure on the gum ridge. Over time, this uneven force can speed up the rate of bone resorption, creating a cycle where the denture fits worse and worse.
Chronic irritation from a poorly fitting denture can lead to oral infections, persistent sore spots, and tissue overgrowth. The WHO reports that oral diseases affect more than 3.5 billion people worldwide and rank among the most common chronic conditions globally. Maintaining a well-fitted denture is one way to stay ahead of preventable oral health problems.
If ongoing tooth pain or swelling develops alongside denture problems, it may signal something more urgent. Knowing when a toothache is an emergency can help you act quickly and protect your health.
When to Consider Dentures vs. Other Tooth Replacement Options
Dentures are not the only way to replace missing teeth, and understanding the alternatives helps you make a more informed long-term decision.
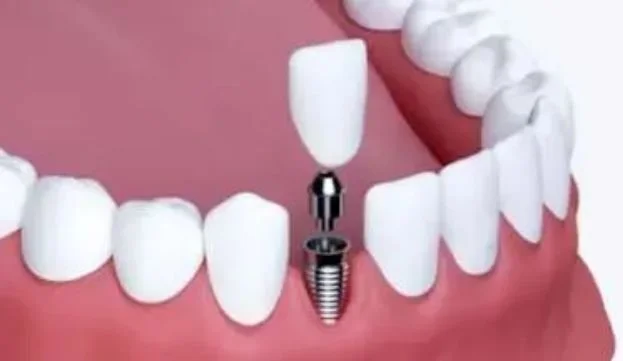
Dental implants are titanium posts surgically placed into the jawbone. They function like natural tooth roots, which means they stimulate the bone and help prevent resorption. The ACP reports that 178 million Americans are missing at least one tooth, and implants have become one of the fastest-growing solutions due to their durability and bone-preserving benefits.
Implant-supported dentures combine the coverage of a full denture with the stability of implants. Because the denture clips onto implant posts rather than resting on the gums alone, it stays more secure and places less pressure on the bone ridge. These tend to last significantly longer than traditional removable dentures.
Bridges are a fixed option for patients missing one or a few teeth. Unlike a removable partial, a bridge is cemented onto the natural teeth on either side of the gap and does not come out for cleaning.
We offer implants, bridges, crowns, and a full range of restorative treatments at our practice. Patients in Cinnaminson, Palmyra, Riverton, Maple Shade, Mount Laurel, and the broader Philadelphia metro area can schedule a consultation to discuss which approach is the best long-term fit.
For patients concerned about how a damaged tooth might affect their denture plan, understanding how dentists decide between a root canal and an extraction can be helpful.
Frequently Asked Questions
How Often Should a Person Get New Dentures?
How often a person should get new dentures depends on the rate of bone change and denture wear. The ADA recommends evaluation every 5 to 7 years. Some patients may need a new set sooner if they experience rapid bone resorption, while others with slower changes may get closer to 10 years from a single denture. Annual checkups allow your dentist to catch fit issues early and recommend a reline or replacement at the right time.
How Many 70-Year-Olds Still Have All Their Teeth?
Very few 70-year-olds still have all their teeth. CDC data shows that about 11% of adults aged 65 to 74 have lost all of their teeth entirely, and the average adult in that age group retains about 22 teeth out of a possible 28 to 32. Complete tooth retention at age 70 is uncommon due to the cumulative effects of decay, gum disease, and injury over a lifetime.
What Type of Dentures Are Most Natural Looking?
The type of dentures that are most natural looking are custom-fabricated dentures made with high-quality acrylic or porcelain teeth and a gum-colored base that closely matches your natural tissue tone. The shape, size, and shade of the teeth are selected to complement your facial features. Implant-supported dentures also tend to look very natural because they sit more securely and do not shift during speaking or smiling.
Will Eating with Dentures Ever Feel Normal?
Eating with dentures will feel more normal over time as the mouth adapts. Most patients find that it takes a few weeks of practice with softer foods before chewing becomes comfortable. The ADA recommends chewing evenly on both sides to keep the denture stable. A well-fitted denture that is regularly evaluated and adjusted makes eating feel as close to natural as possible.
What Is the Average Age People Get Dentures?
The average age people get dentures is typically in the late 40s to early 50s, though it varies widely. CDC data shows that edentulism rises sharply after age 50, increasing from about 6% of adults aged 50 to 64 to roughly 11% of adults aged 65 to 74. Partial tooth loss can occur at any adult age, and younger patients sometimes need partial dentures after trauma or extensive decay.
What Disqualifies You from Getting Dentures?
What disqualifies you from getting dentures includes severe bone loss that cannot support an appliance, active oral infections, and certain medical conditions that impair healing. In most cases, these are temporary barriers. Once infections are treated and the gums are healthy, many patients become good candidates. A thorough dental evaluation determines the best path forward.
Can a Dentist Pull All Your Teeth at Once for Dentures?
A dentist can pull all your teeth at once for dentures in many cases. When full extraction is done in a single visit, an immediate denture is typically placed the same day so the patient is never without teeth. In other cases, extractions are staged over multiple appointments to allow gradual healing. We evaluate each patient individually at our Cinnaminson office. If unexpected pain or swelling develops after extractions, our team provides same-day emergency dental care.
Where to Go from Here
Dentures are a reliable solution for missing teeth, but they are not a set-it-and-forget-it appliance. Regular evaluations, good daily care, and timely relining or replacement keep your dentures comfortable, functional, and healthy for years.
Most dental insurance plans cover a portion of denture services, and we also offer an in-office dental plan for patients without coverage.
If your dentures feel loose, cause irritation, or have not been evaluated in several years, now is a good time to schedule a visit. At Alpha Dental in Cinnaminson, we help patients from Moorestown, Delran, Maple Shade, and across South Jersey keep their smiles strong and comfortable. Call us at (856) 829-1989 to book your appointment.